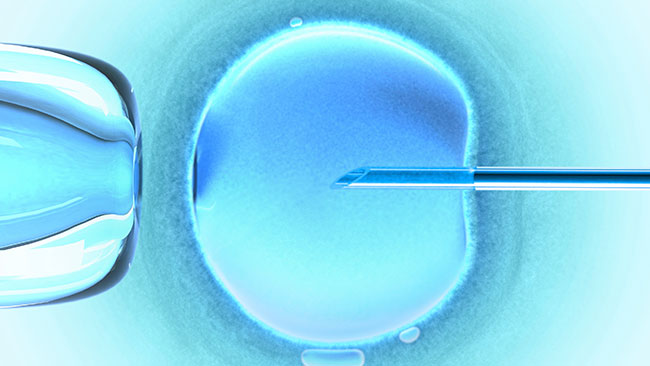
The world of fertility medicine is on the up and up. Couples dealing with the challenges of infertility can be as stressful as having cancer. Fortunately, the latest advances in in vitro fertilization (IVF) are giving them a better chance than ever of achieving their dreams.
What Is In Vitro Fertilization?
IVF is a medical and surgical approach to conception that involves fertilizing eggs outside a woman’s body. Normally, women produce one egg per monthly menstrual cycle, but IVF requires several eggs to increase the effectiveness of each procedure. To boost egg production, women take a series of medications over the course of two weeks.
Mature eggs are then retrieved during a minor surgical procedure in a physician’s office, and fertilized in the laboratory with the partner’s sperm. After about five days, one or two of the developing embryos are inserted into the woman’s uterus or, more and more these days, biopsied, frozen, and saved for future use.
IVF treats infertility caused by various factors, including damaged or blocked fallopian tubes, male problems (such as low or no sperm count), endometriosis, anatomic abnormality, or unexplained infertility. Increasingly, IVF is being used to preserve fertility (through egg and embryo freezing), as well as to diagnose fertility problems.
Advances in IVF
1. Genetic screening. The most important advances in IVF over the past several years involve embryo biopsy and genetic analysis, which help address the challenge of embryos that look good in the lab, but turn out to be chromosomally abnormal. Having too many or too few chromosomes increases miscarriage rates and the likelihood of problems like Down syndrome.
Traditionally, fertility doctors chose the embryos to place in a woman’s uterus according to a grading system based on their appearance. But even top-rated embryos can turn out to have chromosomal abnormalities. Using new techniques, we can now safely biopsy a few cells from each embryo, send them off for genetic screening, and freeze the embryos while waiting for results.
What we learn allows us to then select only chromosomally normal embryos for transfer, rather than relying on their appearance alone. This reduces the risk of miscarriages by about half.
In addition, couples at risk of having a baby with a genetic disease, such as Tay-Sachs, cystic fibrosis, or sickle-cell anemia, may undergo IVF to have their embryos genetically diagnosed and substantially reduce the odds of transmitting the disease to their children.
2. Single-embryo transfer. Another advantage of chromosomal screening is single-embryo transfer, a method that addresses a major criticism of the fertility industry: multiple pregnancy (twins, triplets, or more). For many years, it was standard practice to transfer two or more embryos at a time to maximize the chance of a successful pregnancy. This led to a rise in women carrying multiples, which increases the risk of serious maternal and fetal complications.
Since genetic screening tells us which embryos are more likely to lead to healthy pregnancies and babies, in many cases we can now select just one chromosomally normal embryo to transfer. Research has shown that even women up to age 42 can achieve an approximate 60 percent pregnancy rate with single-embryo transfer — about the same as with two embryos, but with drastically less risk of twins.
3. Frozen embryos. With the shift to chromosomal screening, embryos are increasingly being frozen and then thawed and transferred in a later monthly cycle. In a recent study published in the Journal of Assisted Reproduction and Genetics, my colleagues and I showed that transferring frozen-thawed embryos to a woman’s uterus during a normal monthly cycle is more likely to result in pregnancy and live birth than fresh embryos placed into a uterus stimulated with fertility drugs.
4. New medications. Another IVF advance involves the medication used to increase the production of eggs and speed their maturation. The traditional means of triggering ovulation is through injections of the pregnancy hormone human chorionic gonadotropin (hCG). However, hCG can be problematic for some women, as it sets the stage for ovarian hyperstimulation, a potentially dangerous condition.
As a result, a growing number of fertility centers are moving toward the use of gonadotropin-releasing hormone agonist (GnRHa), which stimulates the brain’s own luteinizing hormones (LH). LH is the body’s natural trigger for egg production. It circulates long enough to ripen and prepare the eggs for harvesting, but not enough to activate ovarian hyperstimulation.
A new study has identified another promising therapy that stimulates the body’s own LH. Researchers found that administering the hormone kisspeptin instead of hCG effectively triggers egg maturation while preventing ovarian hyperstimulation in women at high risk for the condition. Before kisspeptin becomes widely available, however, further research is needed to directly compare it with GnRHa.
The Sooner, the Better
As you can see, several exciting developments are enhancing the success of IVF. However, if you have fertility issues, the best thing you can do to increase your chances of getting pregnant and having a child is to seek fertility counseling earlier rather than later. Since you are born with all the eggs you will ever produce, and the egg supply dwindles as you age, the sooner you seek assistance, the more likely a fertility specialist will be able to help you.
Source: Tanmoy Mukherjee, MD
Associate Director, Division of Reproductive Endocrinology and Infertility,
Mount Sinai Health System;
Co-Director, Reproductive Medicine Associates of New York;
Assistant Clinical Professor of Obstetrics, Gynecology and Reproductive Science,
Icahn School of Medicine at Mount Sinai